Summary of This Article
During pregnancy, mothers may have concerns about the well-being of their baby. Amniotic fluid plays a crucial role in protecting both the mother and the fetus. However, some may not be familiar with its specific functions. In this article, we introduce the concrete roles, components, and structure of amniotic fluid, along with discussing issues related to amniotic fluid. Additionally, we provide explanations about the relationship between NIPT (Non-Invasive Prenatal Testing) and amniocentesis. Please refer to this information for a better understanding.
What is amniotic fluid?
Amniotic fluid is the liquid that fills the uterus during pregnancy. It plays a crucial role in maintaining the environment within the uterus, ensuring optimal conditions for the baby to grow and thrive until birth. In the early stages of pregnancy, amniotic fluid is clear and colorless, but as the pregnancy progresses, it may turn milky due to the baby’s urine production from the kidneys and secretion from the lungs. Additionally, the presence of meconium (fetal stool) in the amniotic fluid can cause it to become cloudy.
The Role of Amniotic Fluid
Amniotic fluid serves the role of protecting the baby from various shocks and stimuli. When the uterus is filled with amniotic fluid, contractions of the uterus help evenly distribute impacts and pressures on the fetus. Additionally, it has a mitigating effect on external temperature changes and maternal conditions, ensuring that the baby maintains a constant body temperature. Amniotic fluid also plays a protective role for the mother by easing pain through its function of preventing direct transmission of fetal movements to the maternal body.
Components and Structure of Amniotic Fluid
The components found in amniotic fluid include various electrolytes, glucose, amino acids, proteins, lipids, urea, uric acid, creatinine, bilirubin, various hormones, growth factors, enzymes, and more. Amniotic fluid contains a diverse range of components necessary for the growth of the baby.
Complications Related to Amniotic Fluid
Amniotic fluid is essential for the healthy development of the baby, but various disorders can lead to complications. Here, we provide detailed explanations of conditions such as polyhydramnios, oligohydramnios, and amniotic fluid embolism.
1.Polyhydramnios
Polyhydramnios is the condition where amniotic fluid is excessively produced. Normally, the amniotic fluid volume gradually increases until around the 34th week of pregnancy and then gradually decreases. The constant regulation of amniotic fluid is maintained as it is produced while the fetus swallows and absorbs it through the gastrointestinal tract. Here, we will introduce the symptoms, causes, and treatment methods of polyhydramnios.
Symptoms
Polyhydramnios often has no symptoms, and some pregnant women may not notice it until diagnosed. However, in severe cases of polyhydramnios, it can lead to difficulties in breathing and early uterine contractions accompanied by pain.
Complications of polyhydramnios include primarily:
- Impending preterm birth due to early uterine contractions
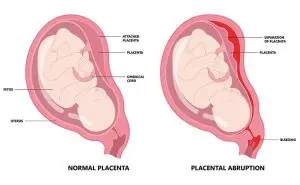
- Premature placental separation after premature rupture of membranes
- Abnormal fetal presentation
- Respiratory difficulties in the mother
- Uterine atony
- Prolapsed umbilical cord
- Postpartum hemorrhage
- Fetal death
Causes
The causes of excessive accumulation of amniotic fluid can be attributed to two main factors: “increased production of amniotic fluid” and “reduced absorption of amniotic fluid.”
Key reasons for the increased production of amniotic fluid include:
- Increased urine production due to maternal diabetes, fetal endocrine disorders, or placental vascular tumors.
Key reasons for the reduced absorption of amniotic fluid include:
- Impaired absorption of amniotic fluid due to congenital abnormalities such as upper digestive tract closure, such as esophageal atresia or duodenal atresia, or functional swallowing disorders.
In addition, leakage of fluid components from the fetus, such as anencephaly, meningomyelocele, or abdominal wall rupture, is also considered a possible cause. More than half of cases of polyhydramnios occur spontaneously and may resolve naturally.
Treatment Methods
In cases where severe pain or early uterine contractions occur, it is necessary to reduce the volume of amniotic fluid. Polyhydramnios can occur spontaneously, resolve naturally, or the cause may remain unknown even after delivery. When polyhydramnios occurs, it is essential to conduct a thorough examination of the fetus, be vigilant for signs of preterm labor, and observe the progression.
In some cases, artificial removal of amniotic fluid may be performed. Currently, there are no strict guidelines regarding the specific volume or rate of amniotic fluid removal, but a method of reducing approximately 1 liter over 20 minutes is often recommended.
2.Amniotic Fluid Embolism
Amniotic fluid embolism is a condition characterized by the blockage of pulmonary capillaries due to the entry of amniotic fluid into the mother’s bloodstream, leading to pulmonary hypertension and associated respiratory circulation disorders. It is typically considered more common in the late stages of pregnancy, but there is also a possibility of occurrence during the 13 to 24 weeks of gestation, particularly in cases of miscarriage. Here, we will introduce the symptoms, causes, and treatment methods of amniotic fluid embolism.
Symptoms
Amniotic fluid embolism generally occurs during or immediately after childbirth. The symptoms mainly include:
- Sudden cardiac arrest
- Sudden difficulty in breathing
- Rapid heartbeat
- Rapid breathing
- Low blood pressure
- Cyanosis
- Hypoxia
- Respiratory failure with intermittent crackles in the lungs
Additionally, as initial symptoms, severe abdominal pain and fetal distress may be observed.
Causes
Factors considered to increase the risk of amniotic fluid embolism include the following symptoms:
- Cesarean section
- Multiple pregnancies
- Maternal aging
- Premature placental separation
- Placenta previa
- Uterine rupture
- Polyhydramnios
- Induced labor
- Forceps delivery
- Abdominal trauma
- Cervical laceration
Not all mothers with these risk factors will necessarily develop the condition. The pathophysiological reasons for why it occurs only in some women are not fully understood, and it is important to recognize that the mentioned risk factors are generally considered possibilities.
Treatment Methods
Supportive therapy is employed to alleviate symptoms in cases of amniotic fluid embolism. This may include transfusions of red blood cells, fresh frozen plasma, and coagulation factors. Ventilatory and circulatory support may be provided, and in some cases, inotropic agents may be necessary. Performing forceps or vacuum delivery promptly after onset may improve maternal outcomes.
3.Oligohydramnios
Oligohydramnios is a condition where the volume of amniotic fluid in the uterus is insufficient compared to the normal amount. The confirmation of amniotic fluid levels is done through ultrasound examinations. To manage amniotic fluid levels, meticulous monitoring and continuous ultrasound assessments are essential. Here, we will introduce the symptoms, causes, and treatment methods of oligohydramnios.
Symptoms
Pregnant women may not experience many noticeable symptoms. The most common sensation is a slight decrease in fetal movements.
Complications of oligohydramnios primarily include:
- Intrauterine growth restriction
- Cesarean section
- Fetal death
Complications that may arise if oligohydramnios occurs from early pregnancy include:
- Limb contractures
- Delayed or incomplete lung maturation
Causes
Factors considered as potential causes of oligohydramnios include:
- Placental insufficiency due to various maternal conditions
- Medications
- Post-term pregnancy
- Fetal kidney disorders causing a decrease in urine production (such as renal agenesis, non-functioning kidneys)
- Intrauterine growth restriction
- Fetal death
- Fetal chromosomal abnormalities
- Rupture of membranes
Treatment Methods
To assess fetal growth, ultrasound examinations are recommended at least every four weeks. In cases of growth restriction, examinations every two weeks are desirable. Amniotic Fluid Index (AFI), which represents the amniotic fluid volume, should be measured at least weekly.
If complications are not present, weekly non-stress tests or fetal monitoring through biophysical profiles, along with delivery around 36 to 37 weeks and 6 days, are recommended.
The relationship between NIPT (Non-Invasive Prenatal Testing) and amniocentesis
Tests such as NIPT (Non-Invasive Prenatal Testing) and amniocentesis are conducted for individuals during pregnancy. Both are essential tests to confirm the health of both the mother and the fetus, but many may not be familiar with the specific differences.
Here, we introduce the roles of NIPT and amniocentesis, serving as a reference for understanding the distinctions.
NIPT (Non-Invasive Prenatal Testing) is a screening test for chromosomal abnormalities
NIPT (Non-Invasive Prenatal Testing) is a prenatal genetic test conducted using the blood collected from the pregnant mother. Since the mother’s blood contains the baby’s DNA, it allows for the screening of fetal chromosomal abnormalities without directly impacting the baby.
NIPT can be performed as early as around the 6th week of pregnancy. However, as it is a screening test, a positive result does not provide a definitive diagnosis. In cases of a positive result, it is recommended to undergo confirmatory testing, such as amniocentesis.
Amniocentesis is a definitive test for chromosomal abnormalities
Amniocentesis is a method for testing chromosomal abnormalities by directly inserting a needle into the pregnant woman’s abdomen to collect amniotic fluid. While it is a highly accurate test, there are associated risks such as infection, bleeding, and amniotic fluid leakage due to the needle insertion into the mother.
Moreover, since amniocentesis requires a sufficient amount of amniotic fluid in the uterus, the test is typically performed around 15-16 weeks of pregnancy. It is known for its high accuracy, nearly approaching 100%. Therefore, if NIPT (Non-Invasive Prenatal Testing) results are positive, undergoing amniocentesis for confirmation is advisable.
At Hiro Clinic, NIPT (Non-Invasive Prenatal Testing) is available for screening chromosomal abnormalities
Amniotic fluid plays a role in protecting both the mother and the baby from shocks and pressure. Troubles related to amniotic fluid include conditions like polyhydramnios, amniotic fluid embolism, and oligohydramnios. Additionally, the relationship and details of NIPT (Non-Invasive Prenatal Testing) and amniocentesis were explained.
At Hiro Clinic, NIPT testing is available, and in the case of a positive result, we can refer you to a partnering testing company for amniocentesis. Since NIPT is a screening test, if a positive result occurs, it is recommended to undergo the confirmatory test, amniocentesis. As NIPT can be performed earlier in pregnancy, having this screening first and subsequently opting for amniocentesis provides reassurance.
【References】
- MSD Manual Professional Version – Polyhydramnios
- Japan Society of Obstetrics and Gynecology – Polyhydramnios
- MSD Manual Professional Version – Amniotic Fluid Embolism
- Japan Society of Obstetrics and Gynecology / Japan Society of Neonatal and Perinatal Medicine – Amniotic Fluid Embolism
- MSD Manual Professional Version – Oligohydramnios
- Japan Society of Obstetrics and Gynecology – Oligohydramnios
- National Center for Child Health and Development – NIPT
Q&A
Amniotic fluid is responsible for protecting the mother and foetus, but some people may not know what it actually does. This article introduces the specific role, composition and structure of amniotic fluid, as well as amniotic fluid-related problems.
-
QWhat can be determined through amniocentesis?Amniotic fluid tests are used to check for chromosomal abnormalities and the risk of foetal damage.
By confirming abnormalities in advance, the test can help you to take early action, such as consulting a genetic counselling specialist or transferring to a specialist hospital where treatment can be provided. -
QHow long does an amniotic fluid test take?The amniotic fluid test itself takes only a few minutes as it only involves collecting amniotic fluid.
However, it may take some time before the sample is taken, as the baby is checked with an echo before the sample is taken.
Also, you will need to rest for 30-40 minutes after the test, so expect the whole process to take about one hour.
Article Editorial Supervisor

岡 博史先生
【役職】
【資格】
【略歴】
【所属】
【SNS】