- What is gestational hypertension?
- Symptoms and complications of pregnancy-induced hypertension
- What is Hiro Clinic NIPT?
- For a healthier pregnancy and childbirth
What is gestational hypertension?
The condition of high blood pressure after 20 weeks of pregnancy is known as gestational hypertension. Previously known as toxemia of pregnancy, the name was changed to gestational hypertension by the Japanese Society of Obstetrics and Gynaecology in 2005.
Hypertension in pregnancy is classified into several categories. Gestational hypertension is the development of hypertension during pregnancy. ‘Pregnancy complicated by hypertension’ if hypertension is present before pregnancy or before 20 weeks’ gestation. ‘Gestational hypertension’ if only hypertension is present after 20 weeks’ gestation, and ‘gestational hypertensive nephropathy’ if proteinuria is also present.
Gestational hypertension occurs in about 1 in 20 pregnant women, but its cause is not understood. However, the disease is more common in cases of high blood pressure, diabetes, obesity and multiple births before pregnancy. As there are few subjective symptoms, it is difficult to check for symptoms of pregnancy-induced hypertension by oneself, and in many cases, pregnancy-induced hypertension is recognised during antenatal check-ups.
Gestational hypertension often becomes severe when it develops at less than 34 weeks’ gestation (premature type). It can cause increased blood pressure, liver dysfunction, kidney and urinary dysfunction, proteinuria, seizures and cerebral haemorrhage in the mother.
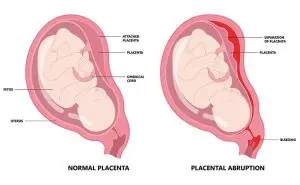
The effects on the foetus include ‘foetal growth retardation’, ‘premature separation of the normal placenta’ where the placenta detaches from the uterine wall and oxygen and nutrients cannot reach the foetus, ‘foetal dysfunction’ and foetal death. For these reasons, gestational hypertension is a very dangerous disease for both mother and child.
The criteria for determining the severity of gestational hypertension by the Japanese Society of Obstetrics and Gynaecology are as follows.
| Minor illness | Serious illness | |
|---|---|---|
| Proteinuria | More than 300 mg/day to less than 2.0 g/day | 2.0 g/day or more |
| Systolic blood pressure | More than 140 mmHg to less than 160 mmHg | 160 mmHg or more |
| Diastolic blood pressure | More than 90 mmHg to less than 110 mmHg | 110 mmHg or more |
Symptoms and complications of pregnancy-induced hypertension
Pregnancy hypertension is considered to have few subjective symptoms. Therefore, there is no reliable way to check for symptoms of pregnancy-induced hypertension. However, in many cases, abnormalities are recognised during antenatal check-ups, so it is important to ensure that antenatal check-ups are carried out during the specified period in order to prevent serious complications.
Symptoms of pregnancy-induced hypertension
●Hypertension ●Proteinuria
Serious complications due to gestational hypertension
●Eclampsia (convulsive seizures) ●Cerebral hemorrhage ●Pulmonary edema ●Impairment of liver function ●Renal impairment
●HELLP syndrome:It is caused by the destruction of red blood cells (haemolysis), a decrease in platelets and impaired liver function. Stomach pain, abdominal pain, nausea and vomiting may occur, and if the disease progresses, the blood may not clot easily and organs throughout the body may be damaged, endangering the life of mother and foetus.
Effects of gestational hypertension on the foetus and cases of caesarean section
A caesarean section is a method of delivery in which the foetus is removed through an incision in the uterus without passing through the birth canal. In many cases, a caesarean section is performed as a rapid delivery when severe complications of gestational hypertension are life-threatening to the mother and foetus.
●Premature separation of the normal placenta: a condition in which the placenta in the uterine wall detaches before birth. The normal supply of oxygen and nutrients to the foetus is not achieved, causing stunting, foetal death or cerebral palsy. Depending on the size of the detached placenta, there may be a risk of haemorrhagic shock to the mother. If the mother’s or foetus’ condition is at risk, a caesarean section is performed.
●Fetal stunting: severe gestational hypertension causes the placenta to deteriorate, preventing the normal supply of oxygen and nutrients to the foetus and impeding its growth. If the foetus’ condition is at risk, a caesarean section is performed.
●Fetal dysfunction: the foetus has or may have future health problems due to impaired respiratory (hypoxia) and circulatory functions. If the foetus’ condition is at risk, a caesarean section is performed.

Who is prone to developing pregnancy-induced hypertension?
Pregnant women who are more likely to develop gestational hypertension often have pre-existing medical conditions such as high blood pressure, diabetes or kidney problems prior to pregnancy. The risk of developing gestational hypertension is also high for pregnant women with infection, first birth, obesity, maternal age over 35 years, multiple pregnancies (twins), pregnant women who have had gestational hypertension in the past and those with a family member with hypertension.
Gestational hypertension is not a very rare condition. However, the causes are still unknown, and regular antenatal check-ups and a diet that prevents high blood pressure are important to prevent pregnancy hypertension from becoming more severe.
Prevention of pregnancy induced hypertension
The causes of gestational hypertension are not understood and medical prevention methods have not been established. However, obesity and infections that predispose to gestational hypertension can be prevented. Prospective mothers should be aware of salt and excessive calorie intake, which can cause high blood pressure, and maintain an appropriate weight through moderate exercise. It is also important to reduce the risk of gestational hypertension by keeping periodontal disease and other infections well treated.

What is Hiro Clinic NIPT?
Hiro Clinic NIPTは、is a NIPT laboratory that performs NIPT with minimal burden on mothers and babies. Each clinic, from Hokkaido to Fukuoka, is staffed by obstetricians, gynaecologists and psychiatrists. At Hiro Clinic NIPT, expert doctors with a wealth of experience and high skills provide appropriate and careful diagnosis.
NIPT at Hiro Clinic NIPT can be performed at 6 weeks and very early pregnancy. The rapid testing by the Tokyo Health Laboratory, which is affiliated with Hiro Clinic NIPT, enables highly accurate detection of the possibility of congenital diseases due to chromosomal abnormalities in the baby, usually within 2-5 days ※1,2 after the blood sample is taken.
※1 Usually within 3-6 days in some clinics and linked facilities
※2 Excluding some plans
Please note that the express delivery option is available at all Hiro Clinic NIPT clinics, excluding collaborating facilities (delivery within 2~3 days of blood collection).
Why Hiro Clinic NIPT results are so fast?
Generally, in NIPT by NIPT laboratories, blood samples (specimens) are taken from the mother and tested for chromosomes at an overseas laboratory. After the blood sample is collected, paperwork is completed and transported, the test is finally conducted and the test results are available. For these reasons, most NIPTs require a period of 5-10 days.
Waiting to find out if the baby has a possible chromosomal abnormality can be a very anxious time for the mother and her family. At Hiro Clinic NIPT , we respect the mother’s and family’s ‘right to know’ more than anything else, and in order to provide NIPT results faster than anywhere else, all NIPT tests are conducted quickly by the Tokyo Health Laboratory in Japan, and 95% of results are delivered within 8 days of the blood being taken (※except for some plans).
The express delivery option is available at all Hiro Clinic NIPT clinics (minimum delivery time of two days after blood collection), except for the collaborating facilities.
NIPT by Hiro Clinic NIPT is also managed by barcode batch management at the time of blood collection. This means that not only is personal information protected, but also there is almost no risk of specimen mix-ups or transport problems.
Hiro Clinic NIPT also offers NIPT for twins
Not many medical centres offer NIPT for twins. Even if they do, many of them only detect 21 trisomy (Down syndrome), 18 trisomy (Edwards syndrome), 13 trisomy (Patau syndrome) in NIPT for twins.
Hiro Clinic NIPT also tests twins for total chromosome heterozygosity and whole-autosomal partial deletions and duplications. Hiro Clinic NIPT also tests for vanishing twins.
※Vanishing twins refers to a condition in which a foetus that died in the early stages of pregnancy is absorbed into the uterus and appears to have disappeared.
What are the miscarriage risks of NIPT?
NIPT differs from conventional prenatal diagnostics such as amniofibroscopy and chorionography in that it does not directly extract amniotic fluid or chorionic villi tissue by injecting a needle into the mother, and is not considered to be directly invasive (damaging) to the foetus.
NIPT is a highly accurate test in which blood is drawn from the mother’s arm and the blood is used to detect the possibility of chromosomal abnormalities in the baby. The risk of miscarriage from amniotic fluid testing is about 0.3%, while the risk of miscarriage from trophoblastic testing is about 1%. NIPT, on the other hand, does not directly invade (damage) the baby, so the risk of miscarriage is almost negligible.
Flow from NIPT to amniotic fluid testing
Mothers considering NIPT often ask: “If I have NIPT, do I need an amniotic fluid test?” We often receive questions such as “If I have NIPT, will I need an amniotic fluid test?
NIPT is a non-confirmatory test to determine whether the baby has any chromosomal abnormalities. The amniotic fluid test, on the other hand, is a definitive test that will tell you whether your baby has chromosomal abnormalities or not.
In most cases, NIPT can be performed from 10 weeks 0 days of pregnancy, while the amniotic fluid test is performed after 15 weeks of pregnancy. Even if NIPT is positive, the amniotic fluid test is not covered by insurance.
Amniotic fluid testing support scheme to subsidise the cost of amniotic fluid testing at Hiro Clinic NIPT
Hiro Clinic NIPT offers a variety of options to reduce the burden on the mother as much as possible.
If you have a positive NIPT result at Hiro Clinic NIPT, we offer an we offer an amniotic fluid test support system that subsidises the cost of the amniotic fluid test up to JPY 200,000 by paying an amniotic fluid test support fee of JPY 3,000 (excluding tax) before undergoing the NIPT test. (tax included) before undergoing NIPT.
Hiro Clinic NIPT can also refer mothers with a positive NIPT test result to a medical institution that offers amniotic fluid testing. Of course, the cost of the amniotic fluid test will be subsidised by the amniotic fluid test support service at the medical institution of their choice. Please note that it is not possible to enrol in amniotic fluid testing support after NIPT has been performed. For more information, please contact the Hiro Clinic NIPT staff.

What is free Hiro Clinic NIPT positive score?
Hiro Clinic NIPT has performed many NIPTs. A vast amount of data on a variety of cases has been accumulated, including NIPT for twins, which could not be carried out at other medical institutions.
Hiro Clinic NIPT provides a ‘Positive Score Report’ , which combines a ‘Positive Score’ and a ‘Positive Concentration Rate’ based on the analysis of these valuable figures, free of charge when 21 trisomy (Down syndrome) and 18 trisomy (Edwards syndrome) are positive.
What is positive score?
The positivity score is a numerical value that measures how far away the NIPT result is from the ‘cut-off value’, which is the boundary value that separates positive and negative results.
The cut-off values are 21 trisomy (Down syndrome), 18 trisomy (Edwards syndrome) and 13 trisomy (Patau syndrome) and whole region partial deletion and duplicated chromosomes, and the further away each number is from the cut-off value, the higher the positive rate.
What is positive target rate?
The positive predictive value is the probability that a positive NIPT result is indeed positive. The positive predictive value depends on the chromosomes examined, and the positive predictive value increases with increasing maternal age.
What is the Hiro Clinic NIPT positive score report utilisation?
he vast amount of data in the Positive Score Report was compiled based on the results of 68,000 tests performed at Hiro Clinic NIPT for NIPT.
The subsequent amniotic fluid test showed that 20 out of 21 NIPT-positive pregnant women were diagnosed with 21 trisomy (Down syndrome), with a 95.24% positive predictive rate, and 9 out of 12 pregnant women were diagnosed with 18 trisomy (Edwards syndrome) with a 75% positive predictive rate. ※As of June 2021
Amniotic fluid testing is a definitive test. However, there is a risk of miscarriage of approximately 0.3% as the test involves the collection of amniotic fluid from the mother’s abdomen by a needle. For the health of the mother’s body and the baby, why not have a NIPT by Hiro Clinic NIPT and consider an amniotic fluid test based on the positive score report?
For a healthier pregnancy and childbirth
Pregnancy hypertension can occur in anyone. There is no sure way to prevent it, but it is important to eat a diet low in salt and balanced in nutrition to reduce the risk of high blood pressure and obesity.
Gestational hypertension is not the only risk associated with pregnancy and childbirth. The most common cause of early miscarriage is chromosomal abnormalities in the baby. Both mother and child should have regular antenatal check-ups and correct eating habits to ensure a healthier pregnancy and delivery.
If you have any questions or concerns about NIPT or your baby’s chromosomal abnormalities, please contact Hiro Clinic NIPT.
【Reference】
- Minds guideline library – Guidelines for the treatment of pregnancy induced hypertension
- Navigating a women-friendly workplace that supports pregnancy and childbirth – Gestational Hypertension Syndrome (Gestational Toxicity Syndrome)
- e-Healthnet – Hypertension
- Department of Obstetrics and Gynaecology, Kumamoto University – Diagnosis and management of multiple pregnancies
Article Editorial Supervisor

岡 博史先生
【役職】
【資格】
【略歴】
【所属】
【SNS】